Back
Polycystic Ovarian Syndrome (PCOS) & Endometriosis Symptoms
By Dr. Zarina Vitebsky, DPT, MSPT, PRPC, TPS, LPF, DN on 10/4/2023
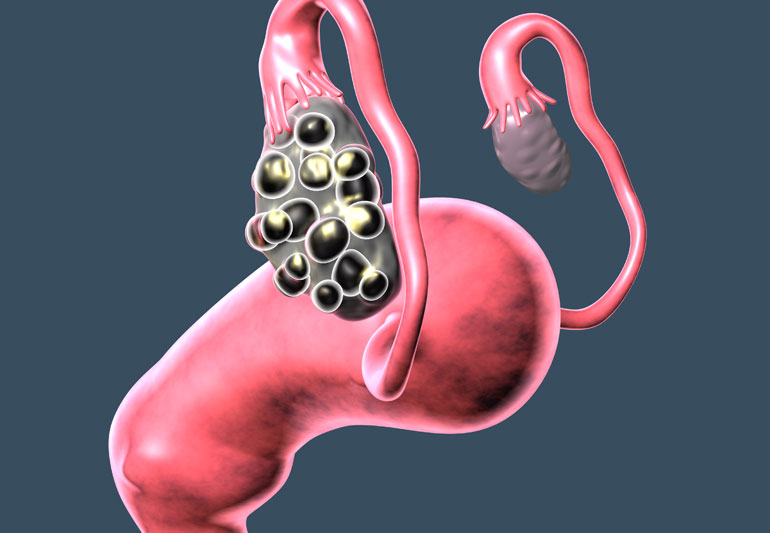
Polycystic Ovarian Syndrome and Endometriosis are two diagnoses that can overlap in symptom presentation but are very different pathologies. The plan of care for these conditions vary greatly! In this blog we’ll learn the differences and similarities, and the course of care for each diagnosis.
A diagnosis of PCOS is confirmed if at least ⅔ clinical presentations exist (this is based off the Rotterdam Criteria which is still has its evidence based limitations): excess androgen activity (i.e testosterone), irregular periods (infrequent or absent ovulation, polycystic ovaries.
Let us break down each characteristic. Excess androgen activity is an increase in hormones (androgens). Androgens (I.e. testosterone) are usually less abundant in women, but are elevated in women with PCOS. Androgen levels can be determined through a blood test. Clinical signs include facial hair growth and acne. Second, people with PCOS have irregular periods and this stems from infrequent ovulation (Oligoovulation) or absent ovulation (anovulation). A third characteristic is polycystic ovaries- as determined by ultrasound. This is visualized as enlarged and higher than normal follicular count in ovaries.
Endometriosis is a disorder where similar tissues inside the uterus start to grow outside the uterine cavity. This lining of the uterus is called endometrium. Its symptoms vary from woman to woman. The severity of pain cannot indicate the endometriosis stage. Diagnosis is confirmed by laparoscopy.
Endometriosis most commonly involves your ovaries, fallopian tubes and the tissues lining your pelvis. With endometriosis, displaced endometrial tissues continues to act as it normally would, therefore it undergoes the process of thickening for a while and eventually breaking down and bleeding during each menstrual cycle. Because this tissue has no way to exit your body, it becomes trapped and causes pain. When it involves the ovaries, cysts called endometriomas can form. The surrounding tissues can become irritated, eventually developing scar tissue and adhesions, which can lead to abnormal bands or fibrous tissue that can cause pelvic tissues and organs to stick to each other.
Here are some common issues women and teens with endometriosis suffer from.
Symptoms:
Pelvic pain during menstrual periods
Pain with intercourse
Pain with bowel movements or urination
Excessive bleeding
Infertility
Other symptoms such as fatigue, diarrhea, constipation, bloating or nausea during menstrual periods
Causes:
Retrograde Menstruation
Transformation of peritoneal cells
Embryonic cell transformation
Surgical scar implantation
Endometrial cells transport
Immune system disorder
Although there is no cure for endometriosis, a variety of treatment options exist.
Treatment for endometriosis is usually either medication or surgery, but this depends on the severity of your signs and symptoms and whether you hope to become pregnant. Generally, doctors recommend trying conservative treatment approaches first, opting for surgery as a last resort.
How Do You Cope with Endometriosis?
Many of us view coping as the ability to overcome problems in life. However, it may be more helpful to view coping as a process made up of a variety of strategies called into play when facing stressful events.
Optimism: Staying hopeful while at the same time realistic about the disease.
Acceptance: Acknowledging that you are experiencing pain is a positive first step in dealing with it.
Tension release: Some may find the need to “let go” or “vent their emotions.” Having a good cry is an example of this strategy. Tension release is used to let out anger, sadness, and despair.
Social support: Seeking out support through groups and from friends, family, doctors, and co-workers.
We believe manual therapy can be hugely beneficial for endometriosis patients, and emphasize the importance of working with other alternative therapies as needed such as acupuncture and pelvic floor physical therapy and managing expectations.
The role of the pelvic floor physical therapist is, therefore, to train you to relax your body and restore balance and alignment. While the pain emanates from the pelvis, the effects of chronic pain are far-reaching due to the role of the pelvic floor in core activities such as movement and coordination.
The therapists at Pelvic Health NJ are able to address not only the pelvic floor dysfunction but also treat the body as a whole addressing the associated functional impairments and symptoms.
Another very important part of pelvic floor recovery is learning techniques to relax the pelvic floor. Manual techniques are directed at loosening and relaxing muscles and relieving abdominal and pelvic pain. The patient is then directed in self-massage and relaxation exercises, which she can continue at home. Visceral manipulation is a key component to add to the treatment of your endometriosis. Organs need to be able to slide and glide - while you are reading this, turn your whole body to the left or right - think of the movement this creates in your abdomen and movement that needs to occur between your abdominal organs to allow this. This freedom of movement is required for everything we do - sitting, standing, walking, running, yoga, lifting, sleeping, breathing etc.
Visceral manipulation is gentle and involves specific techniques aimed at reducing the tension/restriction/adhesion or, on the flip side, improving the mobility between organs. While unfortunately not a cure, it can improve the pain and discomfort you experience by improving the mobility of the tissues affected by endometriosis - for our bodies movement is key!
Treatment of endometriosis should always be a multi-pronged approach addressing lifestyle, medical and individual factors. I believe that physiotherapy plays an important role in helping to reduce your physical symptoms and improving your quality of life.
Visceral manipulation, adhesion release and organ specific fascial mobilization can create more extensibility in fascia/connective tissue around the adhesions associated with endometriosis, which can:
decrease pain (menstrual pain, visceral pain, low back pain and hip pain, pain during sex and digestive pain)
facilitate the expulsion of painful cysts by liberating the uterus from adjacent structures to optimize its function
improve function of the effected organs due to increased mobilization
decrease pain and increase mobility of the surrounding joints and musculature, like the sacroiliac joints, the lumbar spine and hip joints, as well as the associated muscles
mobilize surgical scar tissue, that can often make pelvic pain worse
manage symptoms to maximize time and space between surgery, if surgery is necessary
If you have endometriosis, or are experiencing symptoms (pain during menstruation, pain during sex, painful urination or bowel movements, etc) get yourself rolling and book yourself an appointment.
Please email us at receptionmadison@pelvichealthnj.com or call us at 908-443-9880 to discuss what we at Pelvic Health Physical Therapy can do to help you manage your endometriosis symptoms.
Read More:
Dry Needling for C-Section Scars and Postpartum Recovery By Dr. Christine Martirez PT, DPT on 10/15/2024 Learn how dry needling can be used for c-section scars and c-section recovery How Red Light Therapy Can Be Used to Treat Pelvic Floor Dysfunctions By Dr. Christine Martirez PT, DPT on 10/15/2024 Learn about red light therapy and how it can be used to treat pelvic floor dysfunctions
Are you ready to live pain free?
Request An Appointment