Back
How Does Plantar Fascia Relate to and Cause Pelvic Floor Dysfunction?
By Dr. Zarina Vitebsky, DPT, MSPT, PRPC, TPS, LPF, DN on 9/25/2023
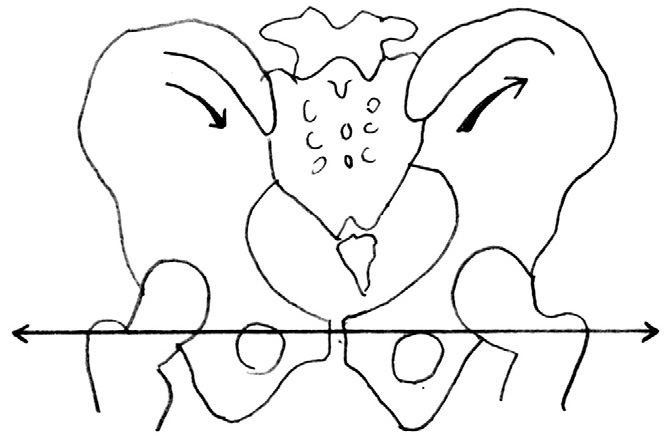
How are the feet related to the pelvic floor?
Plantar fasciitis is inflammation of the plantar fascia (a fibrous web-like connective tissue) due to overload and excessive stress in weight bearing positions (standing, walking, running, jumping). However, the stress is not just stemming from the foot itself, the stress from weight bearing travels up the chain through the knee, hip, and pelvis!
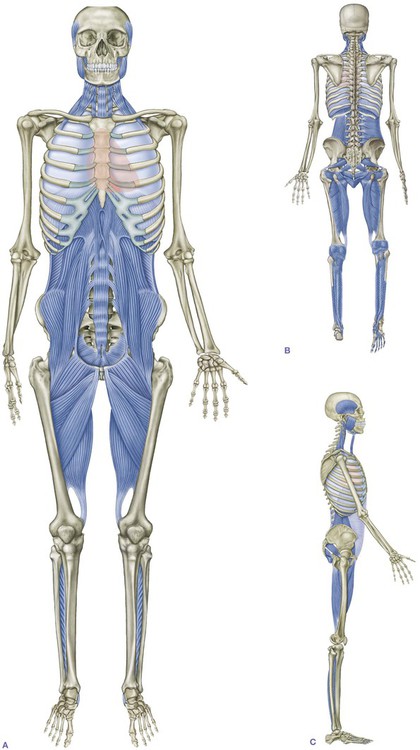
The image above depicts a connective tissue called the deep front myofascial line. One can appreciate the connection from the plantar fascia, on the bottom foot, and how energy can transfer all the way up to the hips and even the base of the skull!
Mechanically, plantar fasciitis is closely associated with collapsed foot arches. With this structural weakening of the foot, the lower limbs have to compensate. The changes and torsions of the lower limb then affect pelvic alignment as seen in the image below.
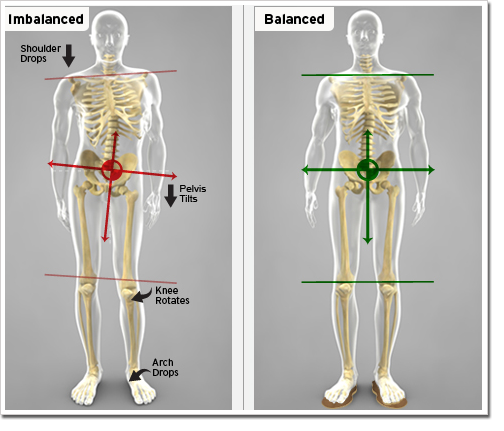
This image depicts how collapsed (pronated) arches can promote tibial torsion and then pelvic torsion.
Here at Pelvic Health Center, you can anticipate a holistic exam of the low back, pelvis, feet and standing posture to assess multiregional involvement! We offer a variety of treatments and recommendations to resolve this issue including:
Deep tissue release work
Footwear modification
Gait retraining
Postural taping
Exercise rehab to improve pelvic stability and efficiency of gait
Working alongside other relevant practitioners (podiatry, chiropractor, and acupuncture)
If you’re experiencing pelvic floor dysfunctions associated with the issues above, including plantar fasciitis, please reach out to us at Pelvic Health Center in Madison, NJ to set up an evaluation and treatment! Feel free to call us at 908-443-9880 or email us at receptionmadison@pelvichealthnj.com.
Works Cited:
Lee JH, Park JH, Jang WY. The effects of hip strengthening exercises in a patient with plantar fasciitis: A case report. Medicine (Baltimore). 2019;98(26):e16258. doi:10.1097/MD.0000000000016258
Read More:
Dry Needling for C-Section Scars and Postpartum Recovery By Dr. Christine Martirez PT, DPT on 10/15/2024 Learn how dry needling can be used for c-section scars and c-section recovery How Red Light Therapy Can Be Used to Treat Pelvic Floor Dysfunctions By Dr. Christine Martirez PT, DPT on 10/15/2024 Learn about red light therapy and how it can be used to treat pelvic floor dysfunctions
Are you ready to live pain free?
Request An Appointment