Back
Understanding Gender Affirming Surgery
By Dr. Zarina Vitebsky, DPT, MSPT, PRPC, TPS, LPF, DN on 7/31/2023
The transgender community is a group of people who identify as a gender different from the sex they were assigned at birth. According to the Williams Institute, an estimated 0.6% of the adult population in the United States identifies as transgender - this translates to about 1.4 million people in the U.S.
It is difficult to calculate the size of the transgender community worldwide because many countries do not collect accurate data for a number of reasons; fear of discrimination, stigmatization, or even persecution are some of the leading reasons for non-disclosure in other parts of the world. However, it is estimated by some researchers that approximately 0.5% of the global population identifies as transgender. Even in the United States, there is no comprehensive data on the number of gender affirming surgeries performed annually. The World Professional Association for Transgender Health (WPATH) estimates that there are thousands of gender affirming surgeries performed annually worldwide.
Gender Confirmation or Gender Reassignment surgeries, as they are commonly known, are medical procedures that alter a person's physical appearance to match their gender identity. There are several different types of gender affirming surgeries that a person may undergo, including surgeries which alter the chest, genitals, and face.
It is important to note that not all transgender persons choose to undergo gender reassignment surgery, and there is no "right" or "wrong" way to identify as transgender. The decision to seek surgical measures is a deeply personal one that should be made by each individual based on their own needs and personal goals.
Vaginoplasty for the Transwoman
Vaginoplasty is a surgical procedure used to create a functional and aesthetically pleasing vagina for transwomen or other individuals experiencing gender dysphoria. It is a complex and specialized procedure that should only be performed by a highly qualified and experienced surgeon.
The specific surgical technique utilized during vaginoplasty will depend on an individual's physical anatomy and their goals for the procedure. The surgery typically involves creating a vaginal canal using skin and tissue from the existing penis and scrotum, and may also include the construction of a vulva and clitoris using skin and tissue from other parts of the body.
Vaginoplasty can be an important and life-changing procedure for transgender individuals who are seeking to align their physical appearance with their gender identity. However, it is a major surgery that comes with risks and potential complications, so it is important for individuals to carefully consider this option and consult with a qualified healthcare provider before proceeding. Recovery from vaginoplasty can take several weeks or longer, and patients may need to abstain from sexual activity for an extended period of time as tissues heal. The diagram below illustrates the steps taken during the vaginoplasty surgery.
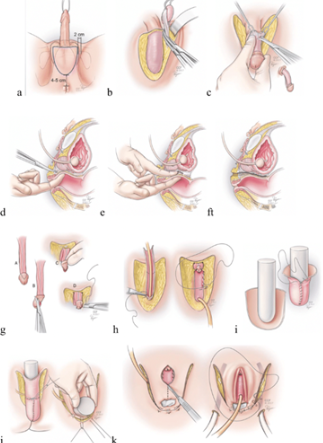
Phalloplasty for the Transman
Phalloplasty is a surgical procedure that involves the construction or reconstruction of a penis. It is typically performed on individuals who were assigned female at birth but identify as male or non-binary, as well as individuals who have suffered a traumatic injury or medical condition that has resulted in the loss or absence of their penis.
During a phalloplasty procedure, a surgeon will typically use tissue from the patient's own body, such as skin, muscle, or fat, to create the penis. The procedure can be performed using a variety of techniques, including free flap phalloplasty, radial forearm phalloplasty, and anterolateral thigh phalloplasty. The choice of technique depends on the individual's anatomy and specific goals for the procedure.
Phalloplasty is a complex and often lengthy procedure that typically requires multiple surgeries and a significant amount of recovery time. It may also involve additional procedures, such as urethral lengthening or scrotal reconstruction, to achieve a more realistic and functional appearance. It is important to note that phalloplasty is a major surgical procedure with potential risks and complications, and should only be considered after careful consultation with a qualified surgeon.
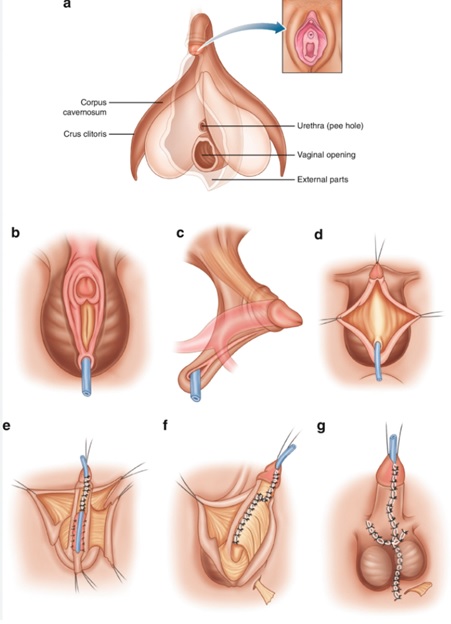
Mastoidoplasty and Metoidioplasty for the Transman
Not to be confused with each other, a mastoidoplasty and metoidioplasty
are two separate surgical procedures performed on different parts of the body during the gender-affirmation process for transmen.
Mastoidoplasty is a surgical procedure that is used to create a more masculine appearance around the mastoid process (the bony area behind the ear) The procedure involves removing excess tissue from this or another part of the body and reshaping the area behind the ear to create a more masculine contour below the ear and behind the jawline. This is more of an aesthetic surgery that can occur as part of a larger gender confirmation surgery, and is typically performed by a plastic surgeon with experience in gender-affirming operations.
Metoidioplasty, on the other hand, is often incorporated as part of the main phalloplasty procedure during lower-body gender confirmation. This procedure involves creating a longer penile shaft (about 4 to 6 cm) by cutting ligaments around the erectile tissue (clitoris) and releasing it from the pubis. During this procedure, the urethra is also lengthened and incorporated into the penile shaft.
As with all of the surgeries discussed on this page, these are major surgical procedures that come with their own risks and complications, and should only be considered after careful consultation with a qualified surgeon.
If you’re experiencing pelvic floor dysfunctions, please reach out to us at Pelvic Health Physical Therapy Center in Madison, NJ to set up an evaluation and treatment!
Feel free to call us at 908-443-9880 or email us at contact@pelvichealthnj.com.
Read More:
Fascial Counterstrain of the Musculoskeletal System By Shannon Strauch, PTA, STMT-1 on 10/21/2024 How treating cartilage and fascia can help reduce joint pain and improve organ function The Impact of Long-Distance Cycling on the Pelvic Floor: Pudendal Nerve and Pelvic Dysfunction By Dr. Christine Martirez PT, DPT on 10/18/2024 Learn how long distance cycling can impact the pelvic floor
Are you ready to live pain free?
Request An Appointment